Curricular Innovation
Read the story of the UW PharmD curricular innovation. 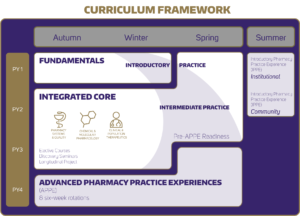
Designing the Provider-Ready Curriculum
Last week’s all-school faculty meeting marked an important shift into our next phase: course design and development. Faculty will begin this work at two all-day retreats later this month.
New Framework Guides our Workgroups
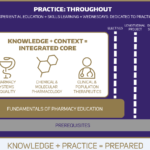
The School of Pharmacy faculty approved the new curricular framework in May 2017 (see Figure 1). Since then, Curricular Innovation Design Workgroups, involving faculty, curricular staff and many alumni and practitioners, have been meeting to add detail to the curricular framework.
Data Analysis Phase

UWSOP Curricular Guidance Team member Dr. Katie Headrick Taylor, from the UW College of Education, led the guidance team in several exercises and facilitated discussions on how people learn best.
New Framework Approved!
After a series of roundtable discussions within our three Departments, and following the May 25, 2017 All-School Faculty and Staff meeting, we are pleased to announce that the faculty of the UW School of Pharmacy have approved a framework for the new curriculum!
Gathering Insights Across Departments

In mid-April, Peggy Odegard shared the Curricular Innovation Framework Proposal with the School of Pharmacy Executive Committee, for distribution by the Department Chairs to the faculty. For the rest of April and into May, faculty in all three departments—Medicinal Chemistry, Pharmaceutics and Pharmacy—reviewed the proposed innovation, asked questions, and offered feedback on the curricular model.
Engaging Our Practice Partners

Members of the CI team, led by Jennifer Danielson, met for a “meeting of the minds” in with several of our stakeholders in practice, including local preceptors who work with our students (and who are future employers of our graduates).
Defining Core Curriculum

In early April, the goal of our meeting was to further define a set of recommendations for the core curriculum, including outlining recommendations for guidance in implementation of any changes.
Defining the Husky Pharmacist

Who is the pharmacist we are graduating? This question led to the development of the Husky Pharmacist document, which includes a list of attributes a pharmacist provider needs to have. The word “provider” is a key feature in the development of our new curriculum, and as a School, we wanted to ground ourselves in a common language around this important term.
Integrating Coursework and Experiential Learning

From February to mid-March, the Curricular Innovation team took stock across teams to better integrate coursework and experiential education. This included meeting with student representatives and with Chairs across the three departments of Medicinal Chemistry, Pharmaceutics, and Pharmacy.
Faculty Reviews Working Model for Curriculum

The Curricular Innovation Guidance Team met with School faculty, several PY4 students, guest pharmacists, and staff at an All-School Faculty Retreat for discussion of a proposed curricular model framework.
Curricular Development
The Curricular Innovation Guidance Team is currently synthesizing faculty input and planning another faculty retreat for January 31, 2017, where the faculty, along with guest practitioners, will review a draft framework of the curricular approach, based on the input and priorities identified at the previous retreat and through student input.
Model Design

A Curricular Innovation Faculty Retreat was held in November 2016, with the key goal to engage the faculty in the next key step of the innovation—development of the new curricular model.
Drafting the final curricular blueprint

The Curricular Innovation Faculty Retreat on November 1st was a success thanks to the majority of UWSOP faculty being in attendance. Faculty heard an overview of the work done by the Curricular Innovation Guidance Team since forming, considered our recommendations for moving forward, and provided their feedback and ideas on our work and next steps.
Pulling Together the Experts

When it comes to in-depth knowledge of the UWSOP curriculum, our faculty are the experts. The success of our new curricular framework and model depends on the full involvement and guidance from our talented and knowledgeable faculty members.
Testing the water with a model ship

Modeling a new curriculum using our draft decision rules and criteria will help us identify problems in the process or framework before diving in and building a full scale version.
Building a Seaworthy Framework

Kayaks frequently skim through our region’s waters, including the Lake Washington Ship Canal that runs through the UWSOP’s backyard. Kayaks were first built about 4,000 years ago for subarctic sea hunting and transport by the indigenous Inuit, Yup’ik and Aleut cultures, using wooden or whalebone frameworks covered with stretched animal skins (Wikipedia, 2016).
Brewing and crafting a curriculum

Our region is known for its unparalleled and innovative brewing of coffee, craft beer, and cider. (Even more reasons to come to the UWSOP!) Over the past several months, the UWSOP has been preparing to brew our own unique flavor of unparalleled and innovative pharmacy education.
Envisioning the pharmacist of 2025

What pharmacy care services are provided to patients now? What trends in practice or service provision are anticipated in the future? What are the critical needs for pharmacist education and training?
Learning how people learn (best)

The UWSOP Curricular Innovation Guidance Team had the pleasure of participating in an interactive session on teaching and learning led by our own team member Dr. Katie Headrick Taylor, Assistant Professor at UW College of Education’s Learning Sciences and Human Development Program.
Debrief: May 17th Pharmacy Curricular Innovation Panel

Members of the UWSOP CI Guidance Team shared their thoughts about the Pharmacy Curricular Innovation Panel event on May 17th, where we had the pleasure of hosting and hearing insights from honored guests from four outstanding pharmacy research and teaching institutions. Dr. Tina Brock from the UCSF School of Pharmacy, Dr. Scott Singleton from the UNC Eschelman School of Pharmacy, Dr. Susan Stein from Pacific University School of Pharmacy, and Dr. Gundy Sweet from the University of Michigan College of Pharmacy summarized their institutions’ curricular models
Debrief: themes/thoughts from our neighbors’ visit

Members of the UWSOP CI Guidance Team shared their thoughts from last meeting’s visit from Dr. Michael J. Ryan, Associate Dean for Curriculum, and Dr. Karen McDonough, Second-Year Program Lead from the School of Medicine, and Dr. Joel Berg, Dean of the School of Dentistry.
Borrowing a cup of sugar from our UW neighbors: School of Medicine, School of Dentistry

The UWSOP Curricular Innovation Guidance Team had the pleasure of hearing about the curricular changes undertaken and implemented last year by the UW School of Medicine (UWSOM) and School of Dentistry (UWSOD).
UWSOP and the Future of Pharmacy

As the roles of pharmacists continue to rapidly shift and expand, UWSOP faculty and alumni are leading the conversation in our community and beyond.
